Plantar Fasciitis
Treatment.
If you're struggling with heel pain — especially that sharp stabbing pain when you take your first steps in the morning, at work or even at nighttime — there's a high chance you're dealing with plantar fasciitis.
At General Foot Care, we are recognised as one of the leading clinics in biomechanics and sports injury rehabilitation in Arnold and the wider Nottingham area. Our podiatrists combine advanced gait analysis, podoscope assessment and evidence-based treatment planning to diagnose the root cause of pain and improve long-term performance.
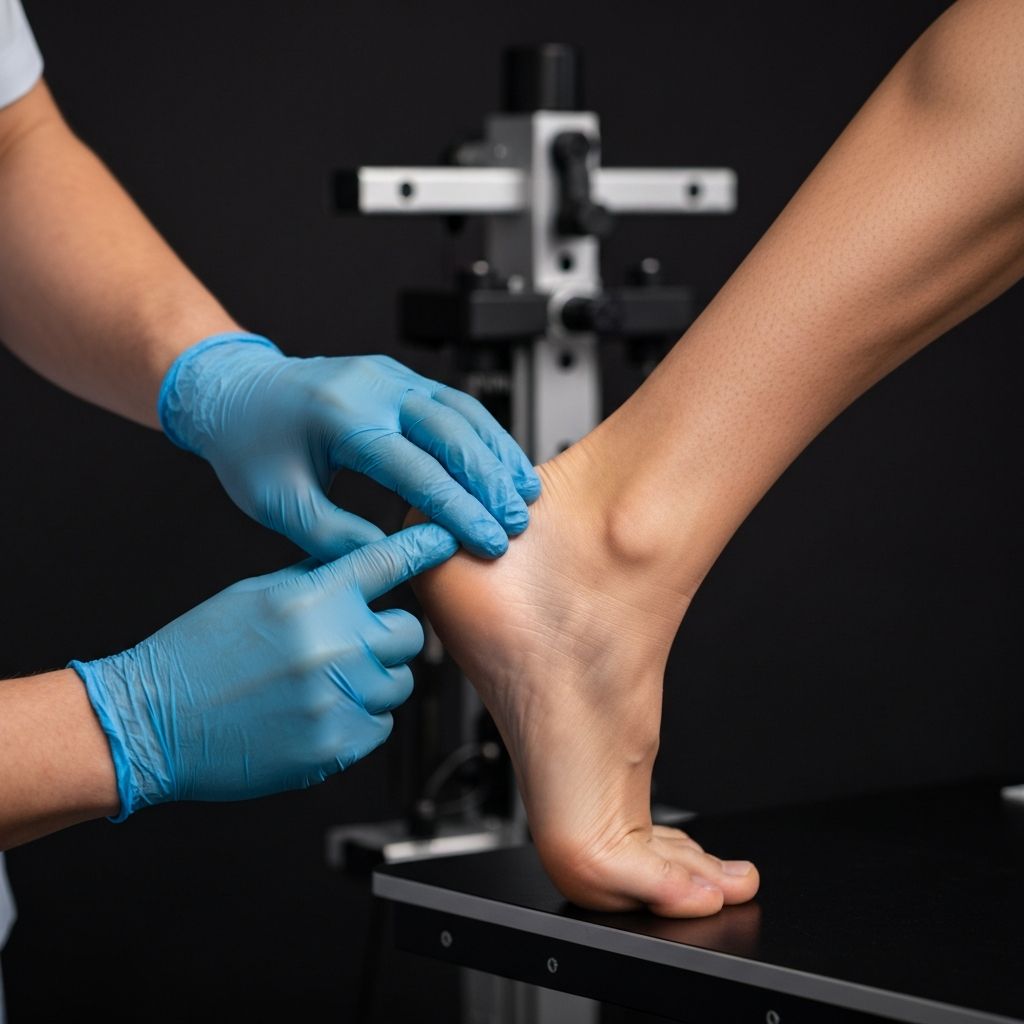
Most people find us after searching:
- "Why does my heel hurt first thing in the morning?"
- "Sharp pain bottom of foot near heel"
- "Plantar fasciitis treatment near me"
- "Heel pain when walking — what do I do?"
- "Why does my arch hurt?"
- "Best insoles for plantar fasciitis"
- "Heel pain came back"
- "Recurring heel pain"
- "Plantar fasciitis flared up again"
If any of these brought you here — you're in the right place. Our specialist plantar fasciitis service combined with advanced biomechanical assessment and gait analysis is the most effective way to diagnose the cause and treat it properly.
Typical Symptoms
Do any of these sound familiar?
Plantar fasciitis is inflammation or irritation of the plantar fascia, a thick band of tissue that supports the arch of your foot. When it becomes overloaded or strained, it causes pain at the bottom of the heel or arch.
Sharp Heel Pain in the Morning
Intense stabbing pain when you take your first steps out of bed — a classic plantar fasciitis sign.
Pain After Rest or Sitting
Heel pain returns when you stand up after sitting or resting for a period of time.
Pain When Walking Barefoot
Walking on hard floors without shoes causes sharp discomfort in the heel or arch.
Pain After Standing for Long Periods
Retail workers, nurses, teachers — anyone who stands all day knows this heel pain well.
Pain During or After Exercise
Running, walking, gym sessions — the heel pain worsens with activity and persists afterwards.
Tight Calves or Arch Stiffness
Reduced ankle mobility, tight Achilles tendon, and stiff foot arch often accompany plantar fasciitis.
What Causes Plantar Fasciitis?
Why you need a biomechanical assessment / gait analysis
Plantar fasciitis can develop for many reasons — and it's almost always the result of a biomechanical imbalance, meaning the way you walk, stand or move is putting excess strain on the fascia.
This is why a biomechanical assessment (gait analysis) is so important — it reveals the exact cause of your pain, so you don't waste money buying different shoes or off-the-shelf insoles hoping something will finally work.
As a leading UK clinic, we offer a full 1 hour 30 minute biomechanical assessment / gait analysis, which includes analysis of foot posture, gait evaluation, podoscope assessment, joint range of motion, muscular strength and flexibility, footwear wear-pattern analysis, custom insole recommendations where needed, and diagnosis based on clinical evidence.
Common causes include:
Evidence-Based Treatment
How we treat plantar fasciitis
Your treatment plan will be tailored to your biomechanical findings and lifestyle. A structured, evidence-based plan used by leading podiatry and sports-injury clinics.
Biomechanical Assessment / Gait Analysis
A comprehensive 1 hour 30 minute assessment including foot posture analysis, gait evaluation, podoscope assessment, joint range of motion testing, muscular strength and flexibility checks, and footwear wear-pattern analysis. This reveals the exact biomechanical cause of your heel pain.
Stretching Programme
We prescribe a tailored stretching programme targeting your calves, plantar fascia and hamstrings. These stretches are essential for reducing tension through the foot and are a cornerstone of effective plantar fasciitis treatment.
Strengthening Programme
A progressive strengthening plan to build resilience in your foot muscles, ankle stabilisers, glutes, hip muscles and core. Weakness in these areas is often the hidden cause of plantar fasciitis in the first place.
Footwear & Activity Advice
We provide expert guidance on correct footwear types, cushioning levels, avoiding aggravating activities, and safe return-to-exercise planning. Small footwear changes can make a huge difference to your recovery.
Custom-Made Orthotics (If Needed)
For patients with significant biomechanical overload, custom orthotics can be life-changing. We use 3D scanning and biomechanics-based design with 3D printing for precision. These orthotics last 10+ years, fit into multiple pairs of shoes, and redistribute pressure to reduce strain on the plantar fascia.
Manual Therapy (If Appropriate)
May include soft tissue mobilisation, joint mobilisation, trigger point work and fascia release techniques to complement your rehabilitation programme.
Structured Loading Plan
We guide you through safe exercise progression, reducing pain without rest-only approaches, and gradually loading the fascia for long-term healing.
Free Follow-Up at 12 Weeks
A free follow-up appointment 12 weeks after your initial assessment to re-evaluate your plantar fasciitis, monitor your improvement, and check whether any adjustments or alterations are needed to your treatment plan or orthotics.

Advanced gait analysis
Video assessment with podoscope, pressure plate and biomechanical evaluation
Why Choose Us
One of the UK's leading clinics for plantar fasciitis treatment
Our patients range from runners to nurses, retail staff to office workers — anyone dealing with persistent heel pain.
- Recognised as one of the UK's leading podiatry and sports-injury providers
- We treat plantar fasciitis every single day
- Advanced gait analysis, podoscope assessment and 3D orthotic scanning
- Evidence-based treatment planning combining stretching, strengthening and load management
- Custom orthotics designed specifically for your biomechanics — lasting 10+ years
- Free 12-week follow-up appointment to monitor your progress
- Steroid injection available if clinically appropriate after assessment
Related Services
Comprehensive lower limb care
Serving patients across Nottinghamshire
FAQs
Your Plantar Fasciitis Questions Answered
Sometimes it can improve on its own, but many cases become chronic if left untreated. When plantar fasciitis becomes long-standing, the healing process slows down significantly, and scar tissue can start to develop around the plantar fascia. This makes the condition more stubborn, more painful, and much harder to treat. Early intervention with a biomechanical assessment gives you the best chance of fast, full recovery.
Not always, but many patients benefit from them if biomechanics are a significant factor. Your podiatrist will assess your foot posture, gait pattern and activity levels during the biomechanical assessment and recommend orthotics only if they are clinically appropriate for your case.
Usually no. We guide you on safe loading so you can stay active. Complete rest is rarely the answer — controlled, progressive loading helps the fascia heal stronger and prevents long-term weakness.
This is classic for plantar fasciitis — the fascia tightens overnight while you sleep, then gets painfully stretched when you take your first steps. This is why morning heel pain is such a strong diagnostic sign.
Not exactly. Heel spurs can occur with plantar fasciitis but are not always the cause of pain. Many people have heel spurs on X-rays but experience no symptoms at all. The pain comes from the inflamed plantar fascia, not the spur itself.
Yes — especially with poor running mechanics, incorrect footwear or sudden increases in training volume or intensity. Runners are one of the most common groups we treat for plantar fasciitis.
Not always. Steroid injections can temporarily reduce inflammation, but they don't fix the underlying cause of your heel pain. Most cases of plantar fasciitis improve with proper biomechanical assessment, footwear correction, strengthening, and load management — without needing an injection. Many of our patients in Arnold and Nottingham recover fully using conservative treatments alone. However, if your assessment indicates that a steroid injection would be clinically beneficial, we do offer this treatment as part of your personalised care plan.
Steroid injections shouldn't be the first option for plantar fasciitis because they mainly mask the pain rather than addressing the underlying cause. While they may offer short-term relief, the effect often wears off, and repeated injections can weaken the plantar fascia. In some cases, this increases the risk of small tears or long-term irritation. If the condition has already become chronic or scar tissue has formed, an injection alone is unlikely to resolve the problem. A proper biomechanical assessment is far more effective, as it identifies the root cause of your heel pain and allows us to create a personalised treatment plan that delivers long-term improvement rather than temporary relief.
Most patients begin to see improvement within 8–12 weeks when following a structured plan. Full recovery varies depending on how long you've had plantar fasciitis, your biomechanics, activity levels, adherence to exercises, footwear, and weight-bearing demands at work. Our job is to give you the quickest, safest and most effective pathway to recovery.
Plantar fasciitis often returns because the underlying biomechanical cause was never addressed. Simply resting, using ice, or taking painkillers masks the symptoms temporarily but doesn't fix the root problem. If your foot posture, gait mechanics, or footwear are still putting excessive strain on the plantar fascia, the pain will return. A biomechanical assessment identifies and corrects these issues to prevent recurrence.
A biomechanical assessment is a comprehensive 90-minute evaluation of how you stand, walk and move. It includes foot posture analysis, gait evaluation, podoscope assessment, joint range of motion testing, muscular strength and flexibility checks, and footwear analysis. Plantar fasciitis is almost always the result of a biomechanical imbalance — meaning the way you walk, stand or move is putting excess strain on the fascia. The assessment reveals the exact cause of your heel pain so we can create a personalised treatment plan that actually works long-term.
Off-the-shelf insoles from the chemist may provide some cushioning, but they are generic and not designed for your specific biomechanics. Many patients waste money trying different insoles hoping something will work. Custom orthotics are precisely designed based on your foot shape, gait pattern and the findings of your biomechanical assessment — which is why they are far more effective for treating plantar fasciitis long-term.
Our clinic is in Arnold, Nottingham. We see patients from across Nottinghamshire including Gedling, Carlton, Mapperley, Woodthorpe, Ravenshead, Hucknall, Daybrook, Bestwood, Calverton, Lambley, Burton Joyce, West Bridgford, Beeston, Bingham, Radcliffe-on-Trent, Mansfield, Newark, Retford, Worksop and surrounding areas.
We are recognised as one of the leading podiatry and sports injury clinics in the UK for biomechanics and plantar fasciitis treatment. Our podiatrists combine advanced gait analysis, podoscope assessment and evidence-based treatment planning to diagnose the root cause of pain and improve long-term performance. We treat plantar fasciitis every single day — from runners to nurses, retail staff to office workers — and our patients consistently tell us we helped them when other treatments failed.
Ready to Get Rid of Your Heel Pain?
Book your biomechanical assessment today and start your journey towards pain-free walking. Same-day and emergency appointments are available — call us or book online.